Dysphagia
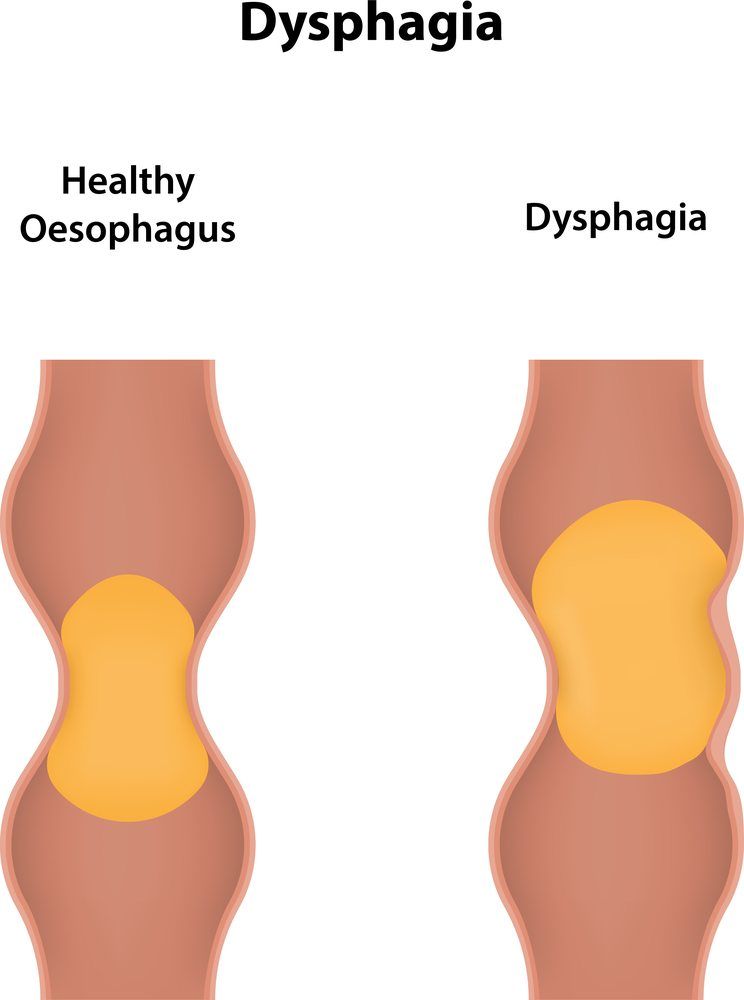
Esophageal dysphagia refers to the sensation of food sticking or getting hung up in the base of your throat or in your chest after you’ve started to swallow. Persistent dysphagia may indicate a serious medical condition requiring treatment.
Did you know…
Although swallowing difficulties can’t be prevented, you can reduce your risk of occasional difficulty swallowing by eating slowly and chewing your food well. Early detection and effective treatment of GERD can lower your risk of developing dysphagia associated with an esophageal stricture.
Frequently Asked Questions
What causes dysphagia?
Swallowing is complex, and a number of conditions can interfere with this process. Sometimes the cause of dysphagia can’t be identified. However, dysphagia generally falls into one of the following categories.
- Achalasia. When your lower esophageal muscle (sphincter) doesn’t relax properly to let food enter your stomach, it may cause you to bring food back up into your throat. Muscles in the wall of your esophagus may be weak as well, a condition that tends to worsen over time.
- Diffuse spasm. This condition produces multiple high-pressure, poorly coordinated contractions of your esophagus, usually after you swallow. Diffuse spasm affects the involuntary muscles in the walls of your lower esophagus.
- Esophageal stricture. A narrowed esophagus (stricture) can trap large pieces of food. Tumors or scar tissue, often caused by gastroesophageal reflux disease (GERD), can cause narrowing.
- Esophageal tumors. Difficulty swallowing tends to get progressively worse when esophageal tumors are present.
- Foreign bodies. Sometimes food or another object can partially block your throat or esophagus. Older adults with dentures and people who have difficulty chewing their food may be more likely to have a piece of food become lodged in the throat or esophagus.
- Esophageal ring. A thin area of narrowing in the lower esophagus can intermittently cause difficulty swallowing solid foods.
- Gastroesophageal reflux disease (GERD). Damage to esophageal tissues from stomach acid backing up into your esophagus can lead to spasm or scarring and narrowing of your lower esophagus.
- Eosinophilic esophagitis. This condition, which may be related to a food allergy, is caused by an overpopulation of cells called eosinophils in the esophagus.
- Scleroderma. Development of scar-like tissue, causing stiffening and hardening of tissues, can weaken your lower esophageal sphincter, allowing acid to back up into your esophagus and cause frequent heartburn.
- Radiation therapy. This cancer treatment can lead to inflammation and scarring of the esophagus.
Dysphagia may be caused by one of many different conditions or illnesses, especially those that weaken the muscles and nerves used to eat and swallow. Some patients develop dysphagia as a result of other disorders like gastroesophageal reflux (GERD).
What are the symptoms of dysphagia ?
Signs and symptoms associated with dysphagia may include:
- Having pain while swallowing
- Being unable to swallow
- Having the sensation of food getting stuck in your throat or chest or behind your breastbone (sternum)
- Drooling
- Being hoarse
- Bringing food back up (regurgitation)
- Having frequent heartburn
- Having food or stomach acid back up into your throat
- Unexpectedly losing weight
- Coughing or gagging when swallowing
- Having to cut food into smaller pieces or avoiding certain foods because of trouble swallowing
How is dysphagia diagnosed?
A general surgeon will likely use a variety of tests to determine the cause of your swallowing problem.
Tests may include:
- X-ray with a contrast material (barium X-ray). You drink a barium solution that coats your esophagus, allowing it to show up better on X-rays. Your doctor may also have you swallow solid food or a pill coated with barium to watch the muscles in your throat as you swallow or to look for blockages in your esophagus that the liquid barium solution may not identify.
- A visual examination of your esophagus (endoscopy). A thin, flexible lighted instrument (endoscope) is passed down your throat so your doctor can see your esophagus.
- Esophageal Manometry. In manometry, a small tube is inserted into your esophagus and connected to a pressure recorder to measure the muscle contractions of your esophagus as you swallow.
- Imaging scans. These may include a CT scan, an MRI scan, or a positron emission tomography (PET) scan.
Will I need Surgery?
Surgery may be recommended to relieve swallowing problems caused by throat narrowing or blockages, including bony outgrowths, vocal cord paralysis, GERD and achalasia, or to treat esophageal cancer.
The type of surgical treatment depends on the cause for dysphagia. Some surgeries that our doctors perform are:
- Esophageal dilation
- Laparoscopic Nissen fundoplication
- daVinci® Anti-Reflux Surgery (Nissen Fundoplication)
- Laparoscopic Heller myotomy
- daVinci® Heller Myotomy (Surgery for Achalasia)


